Medical surgical procedures can be life-saving. But remember, even these cutting-edge medical treatments have requirements patients must meet for them to be safe and effective.
How Do You Know If Surgery Is Safe For You?
Before any surgical procedure, your surgeon evaluates your individual risk for complications – including your medical history, current health conditions, and risk factors – before deciding that surgery is safe. There are some risk factors you can’t change, like if you have a family history of heart disease or if you have type 1 diabetes. One major modifiable risk factor is a person’s weight.

Certain Types of Surgery Are Affected By Obesity
1. Gastric bypass surgery
Gastric bypass surgery is one of the most common weight loss surgeries performed in the United States. The surgery works by reducing the size of the stomach and rerouting the small intestine to bypass a portion of the digestive tract. While gastric bypass surgery is generally safe, there are a number of potential complications that can occur, including infection, bleeding, and blood clots.
2. Gastric sleeve surgery
Gastric sleeve surgery is another common weight loss surgery that involves removing a portion of the stomach. The surgery can lead to a number of complications, including infection, bleeding, and blood clots. Additionally, patients may experience “dumping syndrome,” which is a condition that occurs when food moves too quickly from the stomach to the small intestine.
3. Biliopancreatic diversion with duodenal switch
Biliopancreatic diversion with duodenal switch (BPD-DS) is a more complex weight loss surgery that involves removing a portion of the stomach and rerouting the small intestine. The surgery can lead to a number of complications, including infection, bleeding, and blood clots. Additionally, patients may experience “dumping syndrome” and malnutrition.
4. Laparoscopic adjustable gastric banding
Laparoscopic adjustable gastric banding (LAGB) is a weight loss surgery that involves placing a band around the stomach to create a smaller pouch for food. While LAGB is generally safe, there are a number of potential complications that can occur, including infection, bleeding, and blood clots. Additionally, the band may slip or erode over time, requiring additional surgery to fix.
5. Intragastric balloon
An intragastric balloon is a temporary weight loss device that is placed in the stomach through endoscopy. The balloon takes up space in the stomach so that less food can be consumed at each meal. While intragastric balloons are generally safe, there are a number of potential complications that can occur, including infection, nausea and vomiting, and intestinal obstruction.
6. Aspiration therapy
Aspiration therapy is a new weight loss treatment that involves suctioning food out of the stomach before it can be digested. The procedure is minimally invasive and does not require any incisions or stitches. However, there are a number of potential complications that can occur, including nausea and vomiting, abdominal pain, and diarrhea
7. Hernia Surgery
In hernia repair surgery, obesity greatly increases a person’s chance for complications – as well as the need for a second hernia repair. The general surgeons at USA Hernia Center want the very best for patients – and that means operating at a safe weight where the risk of complications is as low as possible.
“Hernia repairs are technically elective procedures, meaning we want them to be medically optimized in every way. And obesity is one of the main contributing factors for complications in elective procedures,” says Robert Jean, MD, general and trauma surgeon at USA Hernia Center. “Most complications from hernia repair result from a mesh infection. People who are obese are at three times higher risk for a surgical site infection than people who are at a normal or normal-high body mass index.”
Not only does extra weight impact infection risk, it also increases the likelihood that you’ll need surgery again. In the first 6 to 8 weeks after surgery, the hernia repair is relying on a synthetic material to hold the repair together as the scar becomes strong enough to fix the hernia completely.
Why Excess Weight Matters
Increased risk of complications during surgery.
Excess weight can increase the risk of complications during surgery, such as bleeding, infection, and blood clots. Additionally, obese patients are more likely to experience respiratory problems, such as difficulty breathing and pneumonia.
Increased risk of anesthesia-related complications.
Anesthesia is used to prevent pain during surgery. However, obese patients are more likely to experience complications from anesthesia, such as respiratory depression and difficulty waking up from the anesthesia.
Increased length of hospital stays.
Patients who are obese often have longer hospital stays than patients of a healthy weight. This is due to the increased risk of complications after surgery. Additionally, obese patients often require larger incisions, which take longer to heal.
Increased risk of post-operative infections.
Infections are a common complication after surgery, but they are more common in obese patients. This is due to the fact that excess fat tissue can make it difficult for the body to fight off infection
Increased risk of tearing.
Excess weight increases the amount of pressure on the repair, making it more likely to tear. Extra pressure from other factors can also lead to this complication – like smokers who have a chronic cough, people who suffer from chronic constipation, or anyone who is pregnant or planning to get pregnant. The mass of a baby alone is enough pressure on a repair to cause it to fail.
Personalized Risk Analysis
When patients are asked to lose weight, some believe they’ll never be eligible for surgery. Dr. Jean stresses that the goal isn’t to lose 50 percent of their body weight. The surgeons at USA Hernia Center do a risk/benefit analysis for each individual seeking surgery, looking closely to see what changes can be made to ensure the surgery is safe. The effect of excess weight on surgical outcomes is very well studied, and surgical safety calculators demonstrate specifically how weight loss can improve surgical outcomes overall.
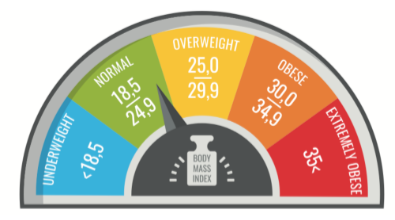
BMI – Body Mass Index
To put it in perspective, a person who has a body mass index (BMI) of 48 may be asked to lower their BMI to between 40 and 45, which translates to a 20 to 30-pound weight loss for most people. And individuals who lower their BMI from 40 to 30 decrease their risk of complications by 50 percent!
When you need a hernia repair – or any surgical procedure – it can be disheartening to hear that you need to lose weight before it’s safe. But you aren’t alone. The USA Hernia Center can connect you with resources and provide information to help you on the path to success. It’s important to remember that no one is being singled out because of obesity, and there are other groups who also receive recommendations about changes that must be made before surgery. Because safe surgery is always the goal.
“Safety is our highest priority, and we ask patients in several situations to make changes that are necessary to reduce their risk of complications. We require heavy smokers to stop smoking. When a person has diabetes or heart disease, we want those conditions under control. Obesity is just a piece of the puzzle, and it’s one risk factor we can control,” explains Dr. Jean. “I know that it’s not easy, but it’s something you can do to increase your chances of a good outcome. I can perform any kind of surgery at any weight, but my question is ‘should I do it?’”
“When I’m having these conversations with patients, I understand that no likes getting advice about how to live their life. We truly want the best for those under our care and want to point them in the right direction,” says Dr. Jean. “Because of the complex nature of hernia surgery and the many factors that contribute to success, preparation at the beginning makes all the difference in the end.”
For more information and services available at University Surgical Associates, visit universitysurgical.com. To schedule an appointment, call 423.267.0466.






It’s so good to know that weight gain raises the chance of surgical complications such as bleeding, infection, and blood clots. Furthermore, you said that obese persons are more prone to have respiratory issues including pneumonia and difficulty breathing. I hope many people get to read this article so they can get all the resources they can have and get necessary bariatric surgery.